My baby has a rash
Rashes are common in newborns and babies. Most rashes are harmless and go away on their own. You may notice that your baby’s skin is dry or peeling in the first 1-2 weeks of life and this is normal.
A common rash seen in babies in the first 3-4 days of life is erythema toxicum. Babies with this type of rash are well in themselves. They have a red blotchy rash that can come and go and often appears on the face, body, upper arms and thighs. This rash does not require any treatment and will go away on its own.
In the first 3 months of life, if your baby has a rash and other symptoms, they may need to be reviewed by a medical professional. Please see below for things to look out for.
|
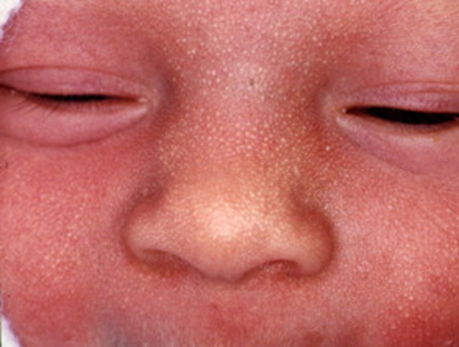
Milia About half of all newborns develop tiny (1-2mm) white spots on their face. These are called milia. These are just blocked sweat pores. They usually clear within the first four weeks of life. |
 |
|
Erythema Toxicum Half of all new-borns develop a blotchy red marks with small bumps and weal’s scattered over face and rest of the body. This is called erythema toxicum. This is usually seen at two or three days old. It's a normal new-born rash that won't bother your baby and clears after a few days. |
|
|
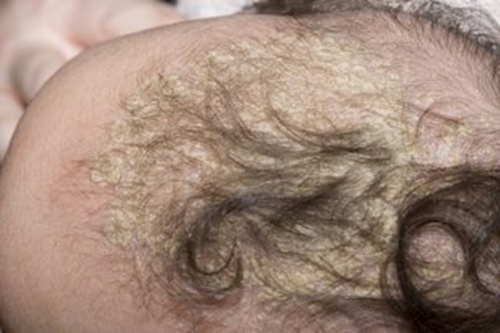
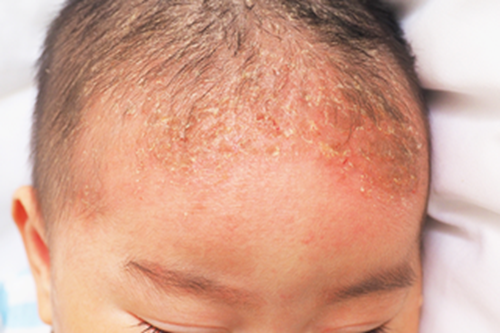
Cradle cap Cradle cap is where yellowish, greasy, scaly patches develop on a baby's scalp. Occasionally, as well as the scalp, the face, ears and neck are also affected
Things you can do to try and get rid of cradle cap:
For futher information see NHS - Cradle Cap |
|
|
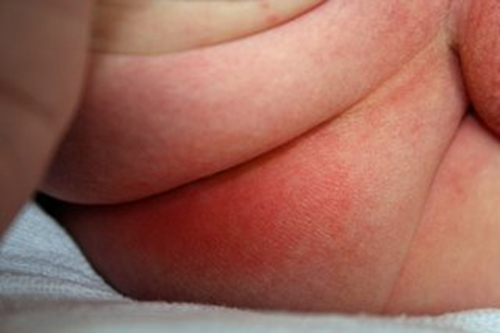
Nappy rash Nappy rash occurs when the skin around the baby's nappy area becomes irritated. It occurs due to a combination of moist environment, chemical irritants and friction.
You can usually reduce nappy rash by taking simple steps to keep your baby's skin clean and dry by frequent nappy changes. If the rash is causing your baby discomfort, your health visitor or pharmacist can recommend a nappy rash cream to treat it. Antifungal cream may be necessary if the rash is caused by a fungal infection. For futher information see NHS - Nappy rash |
 |
|
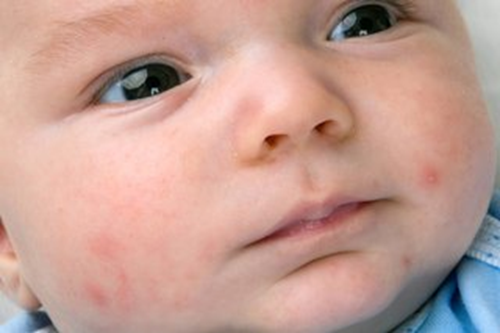
Baby acne (neonatal acne) Baby acne usually develops about two to four weeks after birth. Tiny red or white bumps appear on the baby’s cheeks, nose, and forehead, which may be surrounded by red skin. The cause is unknown. It typically clears up on its own in about three to four months without leaving marks. Regular home care should be enough to treat baby acne:
If you’re concerned that your baby’s acne isn’t going away, your doctor can recommend or prescribe safe treatments |
 |
|
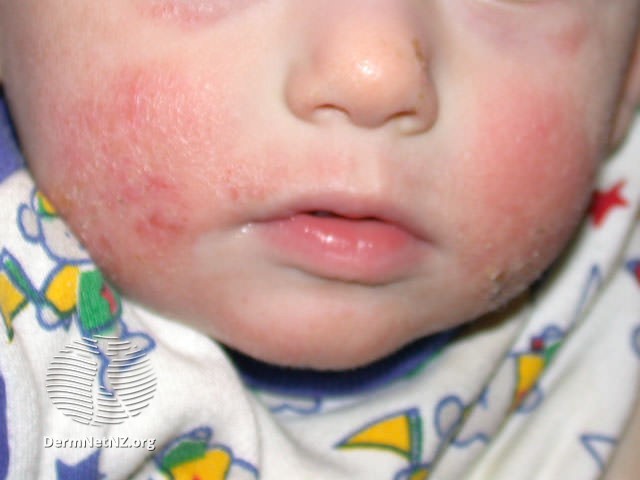
Eczema Eczema is a dry skin condition which causes the skin to become itchy, red, dry and cracked. The most common form is atopic eczema. It mainly affects babies and children but can continue into adulthood. Creams and ointments can often relieve the symptoms. Please see our information on eczema in the dedicated webpage |
photo used with permission from DermNetNZ.org |
|
Sweat rash (miliaria) A heat rash is sometimes called miliaria or prickly heat. It may flare up when your baby sweats. For example, because they're dressed in too many clothes or the environment is hot and humid. It's a sign your baby's sweat glands have become blocked. They may develop tiny red bumps or blisters on their skin, but these will soon clear without treatment. |
More information and pictures of other common skin rashes in babies can be found here.
If you live in Hounslow the key acute NHS provider is Chelsea and Westminster Hospital
Chelsea and Westminster Hospital NHS Foundation Trust - Seborrhoeic dermatitis
When should you worry?
If your child has any of the following:
- A rash that does not disappear with pressure (see the “Glass Test”)
- Becomes pale, mottled or abnormally cold to touch
- Becomes stiff for a prolonged period or has rhythmic, jerky movements of arms or legs that does not stop when you touch it (a fit/seizure)
- Becomes extremely agitated (crying inconsolably despite distraction)
- Becomes floppy or very lethargic (difficult to wake)
- Is going blue around the lips
- Has difficulty breathing
- Is under 3 months of age with a temperature of 38°C / 100.4°F or above (unless fever in the 48 hours following vaccinations and no other red or amber features)
You need urgent help
Go to the nearest Hospital Emergency (A&E) Department or phone 999
If your child has any of the following:
- Has a rash that looks like small blisters or fluid filled spots
- Has broken skin and the surrounding area becomes warm to touch or red. Look out for redness around the base of the umbilicus (belly button) in the first few weeks of life
- Nappy rash that isn’t getting better with simple measures such as regular nappy changes or barrier creams
- Is 3-6 months of age with a temperature of 39°C / 102.2°F or above (but fever is common in babies up to 2 days after they receive vaccinations)
- Continues to have a fever of 38.0°C / 100.4°F or more for more than 5 days
- Becoming increasingly sleepy and not consistently waking for feeds
- No wet nappies in the last 8 hours
- Has a dry mouth or sunken fontanelle (soft spot on the head)
- Is getting worse or you are worried
You need to contact a doctor or nurse today.
Please ring your GP surgery or call NHS 111 - dial 111
If symptoms persist for 4 hours or more and you have not been able to speak to either a member of staff from your GP practice or to NHS 111 staff, recheck that your child has not developed any red features.
None of the above features are present
- It is common for newborns to develop blotchy red skin at 2 to 3 days old. This is a normal newborn rash and shouldn’t bother your baby. It clears after a few days
- Closely monitor your baby for any signs of deterioration by looking out for any red or amber features
- Additional advice is also available for families to help cope with crying in otherwise well babies – click here
Self care
Continue providing your child’s care at home. If you are still concerned about your child contact your Health Visitor or call NHS 111 – dial 111
This guidance was last reviewed 20/12/2024.
For wear and tear, minor trips and everything in between.
Self-care
You can treat your child's very minor illnesses and injuries at home.
Some illnesses can be treated in your own home with support and advice from the services listed when required, using the recommended medicines and getting plenty of rest.
Sound advice
Children can recover from illness quickly but also can become more poorly quickly; it is important to seek further advice if a child's condition gets worse.
For information on common childhood illnesses go to What is wrong with my child?
For wear and tear, minor trips and everything in between.
Self-care
You can treat your child's very minor illnesses and injuries at home.
Some illnesses can be treated in your own home with support and advice from the services listed when required, using the recommended medicines and getting plenty of rest.
Sound advice
Children can recover from illness quickly but also can become more poorly quickly; it is important to seek further advice if a child's condition gets worse.
For information on common childhood illnesses go to What is wrong with my child?
Health visitors are nurses or midwives who are passionate about promoting healthy lifestyles and preventing illness through the delivery of the Healthy Child Programme. They work with you through your pregnancy up until your child is ready to start school.
Health Visitors can also make referrals for you to other health professionals for example hearing or vision concerns or to the Community Paediatricians or to the child and adolescent mental health services.
Contact them by phoning your Health Visitor Team or local Children’s Centre.
Sound advice
Health visitors also provide advice, support and guidance in caring for your child, including:
- Breastfeeding, weaning and healthy eating
- Exercise, hygiene and safety
- Your child’s growth and development
- Emotional health and wellbeing, including postnatal depression
- Safety in the home
- Stopping smoking
- Contraception and sexual health
- Sleep and behaviour management (including temper tantrums!)
- Toilet training
- Minor illnesses
For more information watch the video: What does a health visitor do?
Health visitors are nurses or midwives who are passionate about promoting healthy lifestyles and preventing illness through the delivery of the Healthy Child Programme. They work with you through your pregnancy up until your child is ready to start school.
Health Visitors can also make referrals for you to other health professionals for example hearing or vision concerns or to the Community Paediatricians or to the child and adolescent mental health services.
Contact them by phoning your Health Visitor Team or local Children’s Centre.
Sound advice
Health visitors also provide advice, support and guidance in caring for your child, including:
- Breastfeeding, weaning and healthy eating
- Exercise, hygiene and safety
- Your child’s growth and development
- Emotional health and wellbeing, including postnatal depression
- Safety in the home
- Stopping smoking
- Contraception and sexual health
- Sleep and behaviour management (including temper tantrums!)
- Toilet training
- Minor illnesses
For more information watch the video: What does a health visitor do?
School nurses care for children and young people, aged 5-19, and their families, to ensure their health needs are supported within their school and community. They work closely with education staff and other agencies to support parents, carers and the children and young people, with physical and/or emotional health needs.
Contacting the School Nurse
Primary and secondary schools have an allocated school nurse – telephone your child’s school to ask for the contact details of your named school nurse.
There is also a specialist nurse who works with families who choose to educate their children at home.
Sound Advice
Before your child starts school your health visitor will meet with the school nursing team to transfer their care to the school nursing service. The school nursing team consists of a school nursing lead, specialist public health practitioners and school health staff nurses.
They all have a role in preventing disease and promoting health and wellbeing, by:-
- encouraging healthier lifestyles
- offering immunisations
- giving information, advice and support to children, young people and their families
- supporting children with complex health needs
Each member of the team has links with many other professionals who also work with children including community paediatricians, child and adolescent mental health teams, health visitors and speech and language therapists. The school health nursing service also forms part of the multi-agency services for children, young people and families where there are child protection or safeguarding issues.
School nurses care for children and young people, aged 5-19, and their families, to ensure their health needs are supported within their school and community. They work closely with education staff and other agencies to support parents, carers and the children and young people, with physical and/or emotional health needs.
Contacting the School Nurse
Primary and secondary schools have an allocated school nurse – telephone your child’s school to ask for the contact details of your named school nurse.
There is also a specialist nurse who works with families who choose to educate their children at home.
Sound Advice
Before your child starts school your health visitor will meet with the school nursing team to transfer their care to the school nursing service. The school nursing team consists of a school nursing lead, specialist public health practitioners and school health staff nurses.
They all have a role in preventing disease and promoting health and wellbeing, by:-
- encouraging healthier lifestyles
- offering immunisations
- giving information, advice and support to children, young people and their families
- supporting children with complex health needs
Each member of the team has links with many other professionals who also work with children including community paediatricians, child and adolescent mental health teams, health visitors and speech and language therapists. The school health nursing service also forms part of the multi-agency services for children, young people and families where there are child protection or safeguarding issues.
If you’re not sure which NHS service you need, call 111. An adviser will ask you questions to assess your symptoms and then give you the advice you need, or direct you straightaway to the best service for you in your area.
Sound advice
Use NHS 111 if you are unsure what to do next, have any questions about a condition or treatment or require information about local health services.
For information on common childhood illnesses go to What is wrong with my child?
If you’re not sure which NHS service you need, call 111. An adviser will ask you questions to assess your symptoms and then give you the advice you need, or direct you straightaway to the best service for you in your area.
Sound advice
Use NHS 111 if you are unsure what to do next, have any questions about a condition or treatment or require information about local health services.
For information on common childhood illnesses go to What is wrong with my child?
A&E departments provide vital care for life-threatening emergencies, such as loss of consciousness, suspected heart attacks, breathing difficulties, or severe bleeding that cannot be stopped. If you’re not sure it’s an emergency, call 111 for advice.
Sound advice
A&E departments provide vital care for life-threatening emergencies, such as loss of consciousness, suspected heart attacks, breathing difficulties, or severe bleeding that cannot be stopped. If you’re not sure it’s an emergency, call 111 for advice.