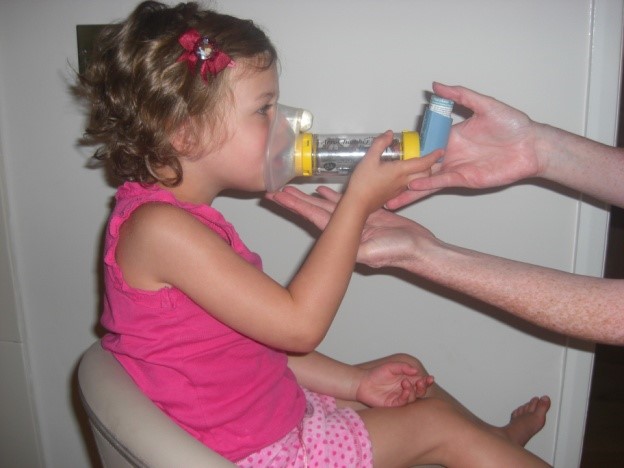
What is an acute exacerbation of asthma?
A worsening of your child’s asthma caused by exposure to one of their triggers. These vary between children but the most common ones are coughs and colds, cold weather, cigarette smoke, pet fur or feathers and pollen.
Asthma Action Plan
Keep this plan with you and take it every time you see the doctor or nurse at your GP surgery (or Hospital). This plan is for patients with asthma – your GP/doctor (or nurse) will fill it in and explain the different medicines to control your asthma. It will also show you how to recognise when the asthma or wheeze is getting worse and what to do about it. By taking steps early – acute attacks can usually be prevented.
Paediatric Pathway
Click here to view the acute asthma paediatric pathway.